Foot pain: causes, exams, treatments
Foot pain is a very common disabling symptom that should not be overlooked. What can she hide? What exams to practice? How to relieve it?
Any foot pain deserves a real clinical examination, carried out by a doctor. Indeed, we must always be able to make a diagnosis, the only guarantor of appropriate care. Do not resign yourself to being in pain, saying to yourself « it’s age » or, in children, « it’s growth » … Making an accurate diagnosis will relieve pain by appropriate treatment « , notes the Dr Thomas-Xavier Haen, orthopedic surgeon in Paris
Foot pain: when to see a doctor?
Bulbs, splinters, and other thorns are generally easy to care for at home. Pain that is moderate, transient, and does not cause significant discomfort usually does not require consultation.
Elsewhere, foot pain is often linked to a pathology purely localized to the feet and benign in the vast majority of cases.
« For the causes which seem obvious (calluses, claw toes, etc.), the treatment passes above all by simple care (pedicuria, chiropody, physiotherapy …). But it is necessary to show them to your doctor first, in order to make sure that this does not reveal a general illness (diabetes, etc.) or a more general problem with posture, and do not simply “do soles” without having identified the cause of the pain, otherwise these Orthopedic insoles are likely to be useless, even harmful. « , insists Dr Haen.
Only a complete medical examination which is not limited to the foot can diagnose the pathology causing the pain. This examination must be methodical:
The interrogation:
• specifies the history;
• takes up the history of pain (mode of onset: trauma, overwork? Nature, location, radiation, hours and evolution of pain. Influence of footwear, cold, etc.)
• research taking medication, some of which may be responsible for foot pain (quinolone, corticosteroids, lipid-lowering agents, etc.);
1/6: PAGE FOOT PAIN
The clinical examination:
• It is comprehensive, both general and local (comparative examination of the 2 feet, study of the gait and the position of the foot resting on the ground);
Additional exams:
• (biological, radiological, etc.) may be prescribed according to the clinical picture.
Foot pain: what can it hide?
Foot pain, even if it seems isolated, can actually integrate into a general pathology which may already be known, or even reveal it. « Foot pain can be a symptom of general illness, projected pain (a back problem) or have a purely local cause. »
A GENERAL ILLNESS AT ISSUE?
Among the most frequent cases we can notably cite:
OBSTRUCTIVE ARTERIOPATHY OF THE LOWER LIMBS (ARTERIES)
It is a frequent pathology in France (800,000 cases), which leads to 5,000 amputations per year. Linked to atherosclerosis, it is favored by the risk factors of atheroma such as smoking and metabolic syndrome (obesity, high blood pressure, high cholesterol, diabetes). The caliber of the arteries is reduced, leading to a decrease in the supply of blood, and therefore oxygen, to the extremities.
What symptoms? Cramps in the calves when walking which reduce the walking perimeter, then at an advanced stage by toe pain in the second part of the night.
DIABETES
It is frequent and threatens the future of the feet because of its complications which are:
• arteritis of the lower limbs;
• diabetic neuropathy, which affects the sensitive nerves (loss of sensitivity, pain, tingling, burning or electric current) and the motor nerves. Note that the motor impairment causes muscle loss, sagging of the foot, deformities (hollow foot, claw toes …), and changes the static of the foot (hyper-support areas with calluses, crevices, etc.). « The diabetic must absolutely pay attention to the care of his feet. Because the loss of sensitivity which prevents him from feeling the wounds of the feet, associated with the poor healing of wounds, can lead to serious infections, sometimes to amputations », recalls Dr Haen;
• gout, because it can be associated with a metabolic syndrome (obesity, high blood pressure, high cholesterol, diabetes), a major cardiovascular risk factor to be taken care of UnmuteLoaded: 0%
2/6 PAGE FOOT PAIN
A back problem at issue?
Foot pain can also be projected pain, that is, caused by a general pathology whose birthplace is elsewhere. Spondyloarthropathy, for example, can start with heel pain when you get up…; pain limited to a heel, an uppers, or a toe … may be the only clinical manifestation of sciatica, called « hanging ».
A purely local cause?
It is only after a general examination that it can be said that the cause of foot pain is purely local, even if it is the most frequent case.
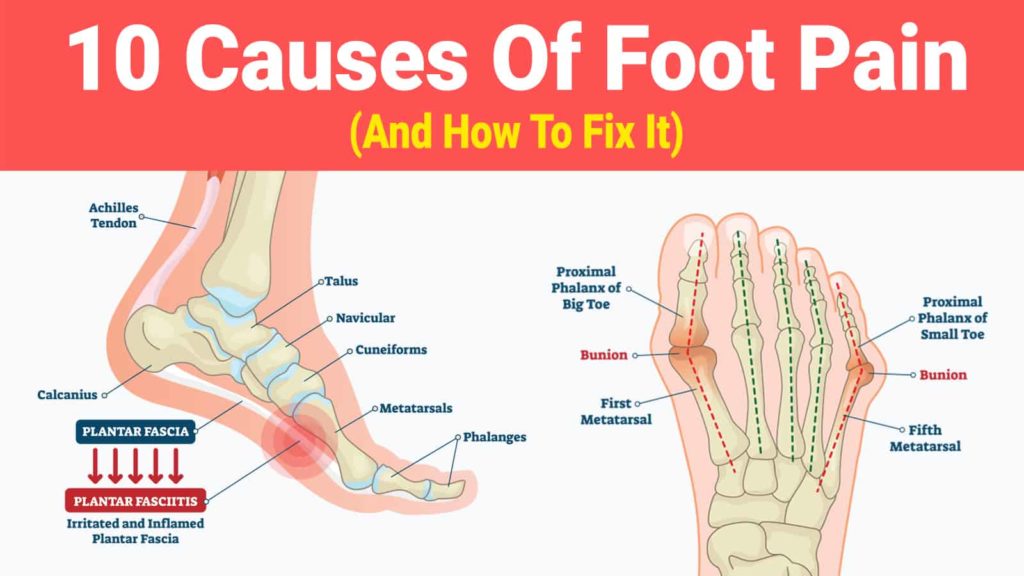
The pathology of the foot is complex. All anatomical structures can cause foot pain (skin, nails, muscles, tendons, bones, joints, arteries, veins, nerves).
The precise diagnosis calls on the general practitioner, if necessary helped by the specialist (rheumatologist, dermatologist, vascular or orthopedic surgeon) or the podiatrist.
Foot pain: what exams?
In the face of purely local foot pain, certain additional examinations may be requested on a case-by-case basis.
• biological examinations;
• looking for signs of inflammation or infection (reactive protein C, blood count);
• research of metabolic anomalies (uricemia, glycemia, calcemia, phosphoremia);
• radiographs, which are almost systematic in podiatry, must always be performed under load (foot in support) to be interpretable;
• ultrasound: to visualize the soft parts (in tendonitis, sprains, etc.);
• on a case-by-case basis: CT or MRI;
• footprint by podoscope at the podiatrist.
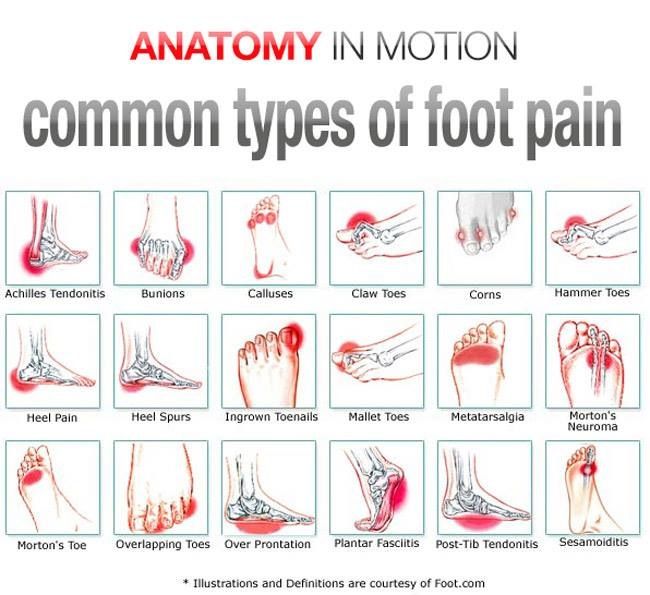
Heel pain
THE Tendency of the Achilles Tendon
Inflammation of the Achilles tendon, common, creates pain in the lower part of the calf and the back of the heel.
Which treatments?
• in the case of a hollow foot: podiatric treatment (soles) and flexibility of the calf by a physiotherapist
• in the case of an athlete who has forced too much: physiotherapy (massages and flexibility exercises), adaptation of the sport (stretching well) and wearing shock absorbing heels. « Beware of cortisone infiltration, which unlike other tendons, can here promote the rupture of the Achilles tendon. Infiltrations are reserved for very specific cases, to be discussed with the sports doctor or surgeon. « says Dr. Haen.
3/6 PAGE FOOT PAIN
THE UNCOVERED BREAK IN THE ACHILLIAN TENDON
« Let us beware of this pain in whiplash in the heel with cracking of the ankle during a brutal impulse (running, squash), to the resumption of sport after 50 years », underlines Dr Haen. If the patient believes that he has had an « ankle » or « sprain » or that he is not properly examined, the risk is to treat with a simple splint, 15 days, whereas it would take real immobilization or even surgical repair. The two ends of the tendon will then continue to move apart, making the situation worse. « In practice, the diagnosis is often corrected by a physiotherapist, who addresses the patient to us urgently, noting a persistent lameness 1 to 2 months after the accident, with his foot dragging on the ground when walking. The longer the patient delays in consulting, the more delicate the reconstruction surgery, « he invites to remember. The diagnosis of Achilles tendon rupture is based on an easy-to-perform clinical examination (Thompson test), but you still have to think about looking for it.
Which treatments? Surgical suturing, or immobilization (3 weeks of resin boot relayed by 3 weeks in a walking boot). In all cases, plan for several months of rehabilitation.
Pain in the forefoot
The HALLUX VALGUS (OR « ONION »)
It is a deviation outside the base of the big toe favored by pointed shoes, in predisposed patients (hereditary factors with early familial forms). In advanced stages, the pain causes the support to be transferred to the other toes (which in turn are painful and deform).
Which treatments? Orthoses (silicone retractors) can be useful in moderate forms. Surgery is not indicated as long as the gene remains purely cosmetic (even if the minimally invasive percutaneous approach limits the surgical risk). It is discussed when debilitating pains appear and inability to put on shoes properly.
THE HALLUX RIGIDUS
It is arthrosis of the big toe (metatarsophalangeal joint). The toe becomes stiff and painful when walking.
Which treatments? Wearing wide shoes with rigid soles and cortisone infiltration. If this fails, surgery can remove the parrot beaks that stiffen the joint, or in an elderly patient, merge the joint to remove the pain.
THE CLAW TOE
This deformation of the toe (often the 2nd toe), in the form of a claw, is frequent and disabling. It gladly touches the elderly subject. The deformed toe presses on the inside of the shoe. A horn is formed above the toe, a callus below, relieved by podiatry care. The abnormal flexion of the toe, initially flexible and reducible, becomes irreducible and prevents putting on.
Which treatments? A silicone orthosis can straighten the toe, physiotherapy can soften it; otherwise surgery is discussed according to age (tendon transfers or shortening of the toe).
4/6 PAGE FOOT PAIN
MORTON’S NEVROME
The shoe compresses a small interdigital sensory nerve downstream between two toes, causing pain and burning sensations, first in some tight shoes, then in all types. The diagnosis is made on clinical examination, confirmed by MRI or ultrasound. The nerve appears thickened on these exams, a witness to his suffering, but it is not a tumor, contrary to what the term neuroma might suggest.
What treatment? Loose shoes and cortisone infiltration on contact with the nerve calm inflammation; otherwise surgery (on an outpatient basis) is discussed.
METATARSALGIA
They give pain in the forefoot (burning, very uncomfortable feeling of « gravel in the shoe ») under the joint of the metatarsals (long bones of the forefoot) with the toes. The systematic wearing of heels favors these pains.These constraints not foreseen by the anatomy of the foot accumulate when walking the weight of the body on the heads of some metatarsals. Other causes can cause such an overload on the metatarsal heads: hollow foot (too arched), load transfer to the outer edge of the foot due to a hallux valgus etc …
Which treatments? Orthopedic insoles; more rarely percutaneous surgery (to shorten a long metatarsal and restore normal foot support).
THE FATIGUE FRACTURE OF A METATARSIAN
It creates significant pain in the forefoot, often in a vitamin D deficient, inactive, who suddenly works a lot. The fracture may go unnoticed at first on the X-ray. Examinations: ultrasound, CT or MRI and a vitamin D test
Which treatments? Put at rest of the foot, these pains always end up healing (in a few weeks).
THE FATIGUE FRACTURE OF A METATARSIAN
It creates significant pain in the forefoot, often in a vitamin D deficient, inactive, who suddenly works a lot. The fracture may go unnoticed at first on the X-ray. Examinations: ultrasound, CT or MRI and a vitamin D test
GLOBAL FOOT DEFORMATIONS
The flat feet (sagging feet) and hollow feet (very arched feet, on the contrary) give support defects and very localized massive load transfers, so calluses under the soles of the feet.
What treatments? soles to lessen the shocks, but especially to straighten the foot and physiotherapy to keep the flexibility of the foot, prevent pain, and relieve (massage inflammatory tendons).
5/6 PAGE FOOT PAIN
Ankle pain
Pains over the foot are rare, can be observed in the hollow foot in particular (tensions above the arch)
INTERNAL EDGE OF THE ANKLE
Very often this pain is related to a flat foot which spreads, sags, creates a tendinopathy of the posterior leg which tries to support the foot, but ends up breaking.
What treatment? soles (to support the foot, relieve the tendon), and physiotherapy (to reduce inflammation).
EXTERNAL ANKLE EDGE
Here the hollow foot, too arched and twisted, leads to tendonitis of the fibula externally, behind the malleolus.
What treatment? soles and physiotherapy.
ANKLE WRAP: CONSULT!
Any sprain must be examined, looking for a fracture, rupture of a tendon, etc .. « If it is still impossible to take support on the foot 7 days after the accident, it is necessary to make a scanner quickly, to find a fracture that went unnoticed on the radio, « said Dr. Haen. « In the event of a fracture, it is necessary to immobilize quickly, otherwise the bone risks badly being welded. And in the event of surgical indication (fracture with displacement), it must be done within 15 days after the accident, otherwise the bone can start to weld in the wrong position, « he adds.
• Interview with Dr Thomas-Xavier Haen, foot, hip and knee surgeon at Clinique Jouvenet (Paris).